Digital Magazine
Digital Magazine
Digital Magazine
"CDOCS Came to the Rescue" - A CEREC Journey
Digital Magazine
Full Mouth Rehabilitation
Digital Magazine
Connecting the Patient to Financial Assistance
Digital Magazine
Milling and Post-mill Processing of 3M Chairside Zirconia
Digital Magazine
The Key to Higher Case Acceptance
Announcements and Feedback
The Vantage Point II
Digital Magazine
Revolutionizing Practices Using Digital Dentistry: Part 3
Digital Magazine
Revolutionizing Practices Using Digital Dentistry: Part 2
Digital Magazine
Revolutionizing Practices Using Digital Dentistry: Part 1
Digital Magazine



 By CDOCS Staff
By CDOCS Staff

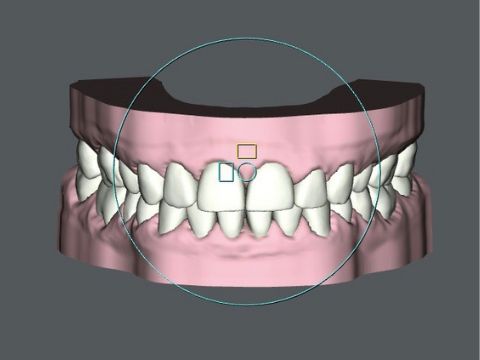
 By Shivi Gupta
By Shivi Gupta
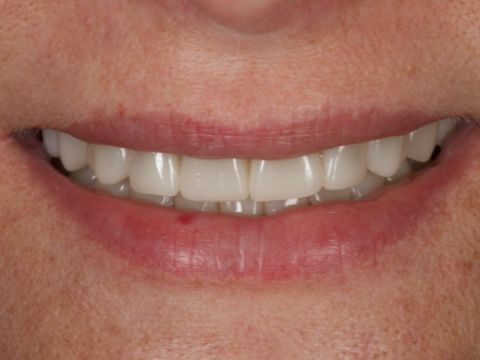
 By Erin Green
By Erin Green

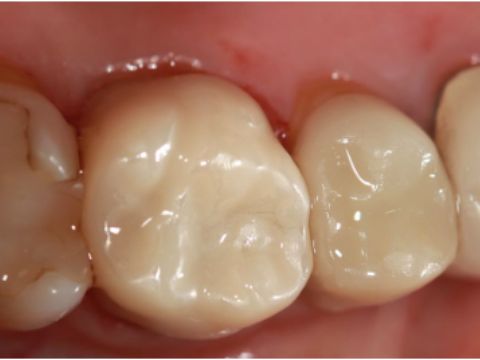
 By Michael Snider
By Michael Snider

 By Matt Jones
By Matt Jones

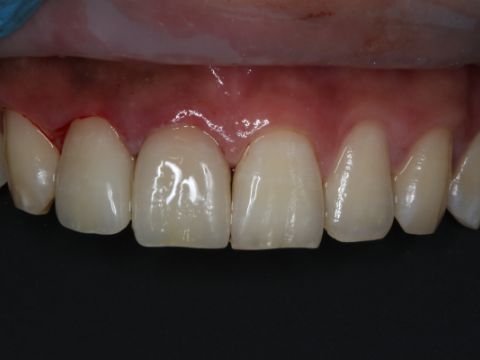
 By Ahmad Al-Hassiny
By Ahmad Al-Hassiny

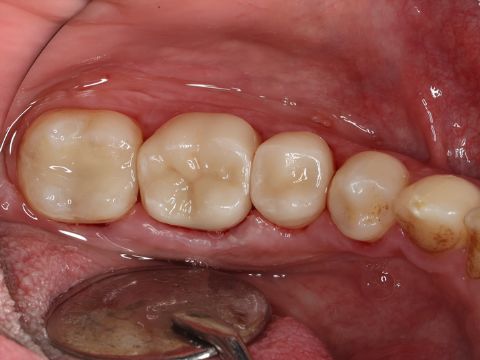
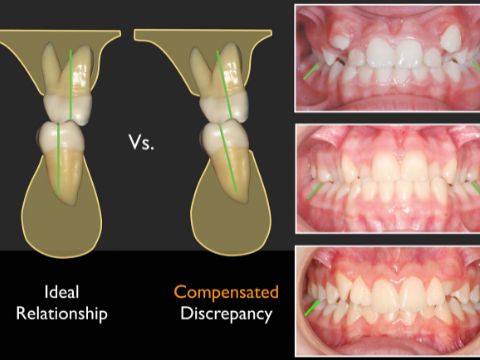
 By Shalin Shah
By Shalin Shah
