Digital Magazine
Digital Magazine
Digital Magazine
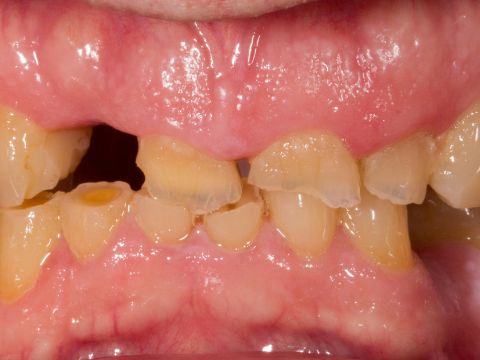
Determining Vertical Dimension for Worn Dentition Case
Case Presentations
Crowns on 8 and 9
Case Presentations
copy and mirror Primescan
Case Presentations
Full Mouth Reconstruction Primescan
Case Presentations
No prep Tetric CAD case
General Discussion
PREOP MARYLAND BRIDGE AND 3D PRINTING
Case Presentations
10 year treatment of a Central Insicor
Case Presentations
3D printing and Essix Retainer
General Discussion
Katana... Thoughts after using it for awhile
Case Presentations
8 Unit Veneer Case
General Discussion


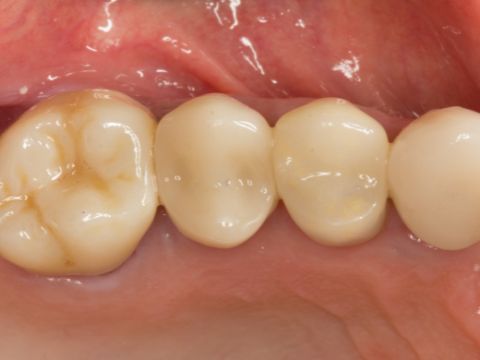
 By Mike Skramstad
By Mike Skramstad